Your Resources
Breast Cancer
Breast Cancer Overview
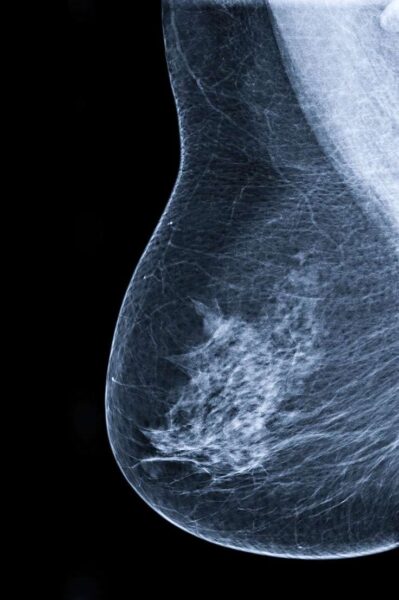
Breast Cancer is the second most common cancer in women. 1One in eight women will be diagnosed with breast cancer in their lifetime. Early detection is key to understanding your risk factors and can help your physician tailor your healthcare to your needs.
Make your health a winning play against breast cancer. Schedule your routine mammogram with your provider today!
_____________
1 https://www.cancer.gov/types/breast
Breast Cancer Video FAQs
Patients with early stages of breast cancer often don’t have symptoms. This makes the need for yearly mammograms and regular self-examinations even more important in order to detect early stage breast cancer. Many of these symptoms can be caused by non- cancerous conditions but it’s important to have any new changes to the breast area checked out by a healthcare provider.
Some symptoms of breast cancer include:
- Lump in the breast or underarm area.
- Enlargement of pores around the breast or nipple area, often described as an orange peel’s texture.
- Dimpling on the breast.
- Unexplained swelling or shrinkage of one of the breasts.
- Inverted nipple.
- Nipple discharge that is clear or bloody.
There are a variety of 2factors that can determine your risk of developing breast cancer, it’s important to know these factors and discuss them with your physician.
- Age: As with many other diseases, your risk of breast cancer goes up as you get older. About two out of three invasive breast cancers are found in women 55 or older.
- Race/Ethnicity: White women are slightly more likely to develop breast cancer than Black, Hispanic, and Asian women. But Black women are more likely to develop more aggressive, more advanced-stage breast cancer diagnosed at a young age.
- Family History: A woman’s risk for breast cancer is higher if she has a mother, sister, or daughter (first-degree relative) or multiple family members on either her mother’s or father’s side of the family who have had breast or ovarian cancer.
- Personal History: Women who have had breast cancer are more likely to get breast cancer a second time.
- Genetic Mutations: Women who have genetic mutations to certain genes, such as BRCA1 and BRCA2, are at higher risk of breast and ovarian cancer.
- Breast Density: Dense breasts have more connective tissue than fatty tissue, which can sometimes make it hard to see tumors on a mammogram. Women with dense breasts are more likely to get breast cancer.
- Radiation to chest or face before the age of 30: If you had radiation to the chest or face to treat another cancer or acne, you have a higher-than-average risk of breast cancer.
- Pregnancy or Breastfeeding History: Breastfeeding can lower the risk of breast cancer if a woman has breastfed longer than a year, and women who have never had children or had their first child after 30 have a higher risk than women who had their children before the age of 30.
- Menstrual and Menopause History: Starting menstrual periods before age 12 and starting menopause after age 55 expose women to hormones longer, raising their risk of getting breast cancer.
- Using Hormone Replacement Therapy: Some types of HRT can increase your risk of breast cancer.
Certain lifestyle behaviors can also affect potential breast cancer risk such as factors relating to weight, smoking, alcohol consumption and exercise habits.
_______________________
2 https://www.breastcancer.org/risk/risk-factors
Early detection is key to improving treatment outcomes and survival rates. Regular self-breast exams and yearly mammograms are the best ways to spot cancer early. Ultrasounds and MRIs may also be used to help confirm the diagnosis.
Once diagnosed, your doctor will discuss treatment options tailored to your specific needs. The treatment plan varies depending on factors like the type and stage of cancer.
At Clearview Cancer, physicians provide personalized care, ensuring the treatment aligns with the guidelines set by the National Comprehensive Cancer Network (NCCN). There are standard treatments currently in use, as well as clinical trials that offer access to new drugs or regimens that aren’t yet widely available. Support groups can also play a vital role in the treatment process and improve overall patient outcomes.
Treatment Options for Breast Cancer:
